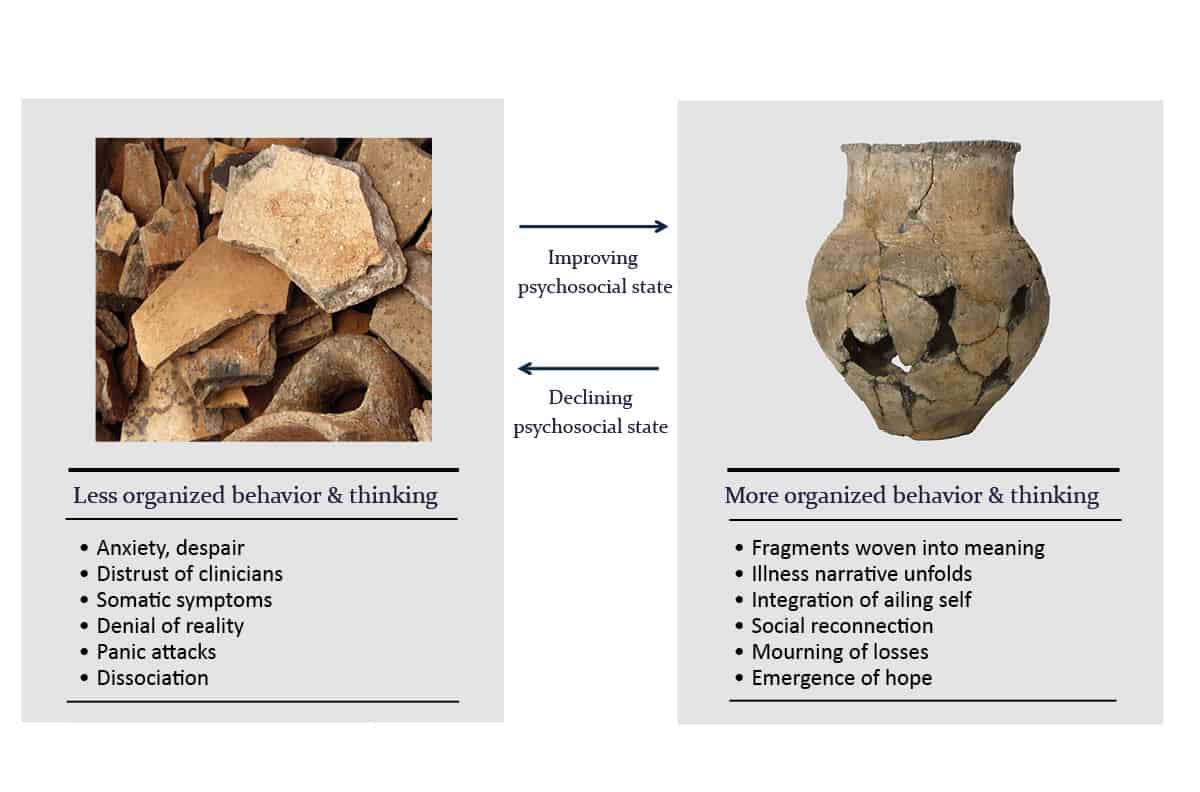
The Trauma of Dialysis Initiation
We are happy to announce that Dr. Gavril Hercz’s article is published, in the Perspective section of JASN October 2017 28: 2835-2837. The link for the article can be found here.
http://jasn.asnjournals.org/content/28/10/2835
“The trauma of dialysis initiation” discusses at length the psychosocial impact of serious medical illness, such as kidney disease, which affects not only patients but also caregivers and clinicians. Although turbulent behaviour may arise, as a consequence of inner conflicts and anxieties, at any time throughout the illness trajectory of the patient, it is appreciated more at the time of dialysis start.
Caring for the physical aspects of illness can be very challenging for clinicians and caregivers and thus, very often, takes the focus away from the emotional and psychological well being of the patient. In an Article: How Technology has impacted the Health Care Arena”, we read how
Clinical practice is increasingly dependent on technology, which has significantly improved the way patients are treated for their illness, resulting in better outcomes. But has it also improved the emotional connection between a patient and his/her clinician?
The dynamics of this emotional turmoil vary from patient to patient and the better understanding of how the disease and the treatments may affect patients and their families differently, will help the clinician to connect with them in a supportive and constructive manner.
In one of our previous posts, Quality of Life Progression during Dialysis Initiation, we discussed that:
Dialysis initiation is often associated with emotional distress, involving both patients and their families. Many aspects of these dynamic changes can be appreciated by evaluating different quality of life (QOL) parameters. Repeating the same measurements over periods of time, in the same patients, can provide useful information on how impactful this period is. As well, focusing on internal and external resources may predict which patients are at greater risk of distress and, more importantly, possible interventions to mitigate these disturbances.
In these studies, Dr. Hercz has shown that patients with greater degrees of resiliency (inner resources) and appreciated social supports (external resources) cope better during these traumatic illness transitions. Finding ways of enhancing both these supports would go a long way to helping patients cope and self-manage better. This remains a challenge for clinicians of all persuasions.
About the Author
admin
We are a community of nephrology and mental health clinicians, patients, families, and caregivers who are committed to understanding and helping people cope with the psychosocial impact of chronic kidney disease.
We are happy to announce that Dr. Gavril Hercz’s article is published, in the Perspective section of JASN October 2017 28: 2835-2837. The link for the article can be found [...]



